Pickering University. Q. Gunock, MD: "Purchase Proventil online - Proven online Proventil".
Comparative evaluation of five diagnostic methods for demonstrating microsporidia in stool and intestinal biopsy specimens cheap proventil 100mcg fast delivery asthma vs allergies. Microsporidia: emerging advances in understanding the basic biology of these unique organisms cheap 100 mcg proventil amex asthma jokes. Improved light-microscopical detection of microsporidia spores in stool and duodenal aspirates discount 100 mcg proventil otc asthma from allergies. Clinical significance of enteric protozoa in the immunosuppressed human population. Eradication of cryptosporidia and microsporidia following successful antiretroviral therapy. Modification of the clinical course of intestinal microsporidiosis in acquired immunodeficiency syndrome patients by immune status and anti-human immunodeficiency virus therapy. Analysis of the beta-tubulin genes from Enterocytozoon bieneusi isolates from a human and rhesus macaque. Analysis of the beta-tubulin gene from Vittaforma corneae suggests benzimidazole resistance. Efficacy of ivermectin and albendazole alone and in combination for treatment of soil-transmitted helminths in pregnancy and adverse events: a randomized open label controlled intervention trial in Masindi district, western Uganda. Usually within 2 to 12 weeks after infection, the immune response limits multiplication of tubercle bacilli. A significant disadvantage of the 9-month regimen is that the majority of patients do not complete all 9 months of therapy. Increased clinical monitoring is not recommended, but should be based on clinical judgment. If the serum aminotransferase level increases greater than five times the upper limit of normal without symptoms or greater than three times the upper limit of normal with symptoms (or greater than two times the upper limit of normal among patients with baseline abnormal transaminases), chemoprophylaxis should be stopped. Factors that increase the risk of clinical hepatitis include daily alcohol consumption, underlying liver disease, and concurrent treatment with other hepatotoxic drugs. Patients should be reminded at each visit about potential adverse effects (unexplained anorexia, nausea, vomiting, dark urine, icterus, rash, persistent paresthesia of the hands and feet, persistent fatigue, weakness or fever lasting 3 or more days, abdominal tenderness, easy bruising or bleeding, and arthralgia) and told to immediately stop isoniazid and return to the clinic for an assessment should any of these occur. The majority of patients have disease limited to the lungs, and common chest radiographic manifestations are upper lobe infiltrates with or without cavitation. If a sensitive broth culture technique is used, the sensitivity of sputum culture is quite high. With progressive immunodeficiency, granulomas become poorly formed or can be completely absent. The yield of mycobacterial urine and blood cultures depends on the clinical setting; among patients with advanced immunodeficiency, the yield of culture from these two readily-available body fluids can be relatively high68,72 and may allow definitive diagnosis and be a source of an isolate for drug-susceptibility testing. In a 2014 meta-analysis, the sensitivity for detection of rifampin resistance was 95% (95% confidence interval 90%–97%) and specificity was 98% (95% confidence interval 97%–99%). Two recent analyses showed that treatment failure was more common among patients whose isolates had phenotypic susceptibility but mutations in the rpoB gene compared to patients whose isolates had normal rpoB gene sequences. Ethambutol can be discontinued when susceptibility to isoniazid and rifampin has been confirmed. Regimens that included once- or twice-weekly dosing during the continuation phase of therapy were also associated with increased risks of treatment failure or relapse with acquired rifamycin resistance. Although drug-drug interaction studies suggest that thrice-weekly and daily rifampin dosing is associated with similar levels of cytochrome P450 enzyme induction when dosed with raltegravir,120 whether there is a difference between daily and thrice- weekly dosing during the continuation phase of therapy has not been adequately studied in randomized trials. Every effort should be made to assure that patients receive daily therapy as previously described, allowing up to 28 weeks to complete at least 24 weeks (6 months) of treatment to accommodate brief interruptions of therapy for management of adverse drug reactions as described below. Addition of a fluoroquinolone may improve outcomes in patients with isoniazid-monoresistant tuberculous meningitis. The mortality was decreased from 13% in the 2-week arm to 8% in the 8-week arm,137 and viral suppression rates were very high among those who survived (>95%). Given the need for the initiation of five to seven new medications in a short time, adherence support should be offered. These drug-drug interactions are complex, but most result from the potent induction by the rifamycin of genes involved in the metabolism and transport of antiretroviral agents. Regular monitoring of transaminases is recommended when double dose lopinavir/ritonavir is used (e. Rifabutin has little effect on ritonavir-boosted lopinavir162 or atazanavir,163 and its co-administration results in moderate increases in darunavir164 and fosamprenavir concentrations. Therefore, the dose of rifabutin must be decreased to avoid dose-related toxicity, such as uveitis and neutropenia. However, given that the risk of adverse events related to high levels of rifabutin’s metabolite with this dosing strategy has not been firmly established, close monitoring for toxicity (especially neutropenia and uveitis) is required until larger studies provide adequate safety data. Raltegravir concentrations are significantly decreased when co-administered with rifampin. A pharmacokinetic study in healthy volunteers showed that increasing the dose of dolutegravir to 50 mg twice a day with rifampin resulted in similar exposure to dolutegravir dosed 50 mg daily without rifampin, and that rifabutin 300 mg daily did not significantly reduce the area under the concentration curve of dolutegravir. The breadth and magnitude of drug-drug interactions between the rifamycins and many antiretroviral drugs can be daunting. Management of Suspected Treatment Failure The causes of treatment failure include undetected primary drug resistance, inadequate adherence to therapy, incorrect or inadequate regimen prescribed, subtherapeutic drug levels due to malabsorption, super-infection with drug-resistant M. Patients with suspected treatment failure should be evaluated with a history, physical exam, and chest radiograph to determine whether the patient has clinically responded to therapy, even though his/her cultures have not converted. The initial culture results and drug-resistance tests, treatment regimen, and adherence should also be reviewed. Serologic testing for hepatitis A, B, and C should be performed, and the patient should be questioned regarding symptoms suggestive of biliary tract disease and exposures to alcohol and other hepatotoxins. Thereafter, if appropriate, relevant antiretroviral drugs and cotrimoxazole may be recommenced. Resistance to rifampin alone, or to rifampin and other drugs, substantially increases the complexity and duration of treatment. In general, such regimens will include a later-generation fluoroquinolone, a second-line injectable agent (i. Whenever possible, treatment should be individualized to the patient’s specific drug-susceptibility testing results or based upon his or her treatment history. An intensive phase of 8 months is then followed by a continuation phase without the injectable agent for an additional 12 to 18 months. Such screening should include serum chemistries, liver function tests, thyroid stimulating hormone, and audiometry. Sputum cultures should be sent monthly, even after culture-conversion, so that any relapse and amplified resistance are detected early. Specifically, efavirenz decreases bedaquiline levels and should not be used concurrently. The condition is thought to result from the recovering immune system driving inflammatory reactions directed at M. This manifests with nausea and vomiting, tender hepatic enlargement, cholestatic liver function derangement, and occasionally jaundice. Many patients require symptomatic therapy (analgesia, anti-emetics), and if symptoms are significant, anti-inflammatory therapy should be considered.
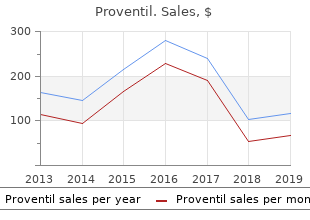
To address the spectrum of substance use problems and disorders order proventil 100 mcg on line definition von asthma, a continuum of care provides individuals an array of service options based on need cheap proventil online amex asthma symptoms blood pressure, including prevention discount proventil 100 mcg without prescription asthma disease, early intervention, treatment, and recovery support (Figure 4. Traditionally, the vast majority of treatment for substance use disorders has been provided in specialty substance use disorder treatment programs, and these programs vary substantially in their clinical objectives and in the frequency, intensity, and setting of care delivery. Substance Use Status Continuum Substance Use Care Continuum Enhancing Health Primary Early Treatment Recovery Prevention Intervention Support Promoting Addressing Screening Intervening through medication, Removing barriers optimum physical individual and and detecting counseling, and other supportive and providing and mental environmental substance use services to eliminate symptoms supports to health and well- risk factors problems at and achieve and maintain sobriety, aid the long- being, free from for substance an early stage physical, spiritual, and mental health term recovery substance misuse, use through and providing and maximum functional ability. Includes through health evidence- brief Levels of care include: a range of social, mmunications and based intervention, educational, • Outpatient services; access to health programs, as needed. This chapter describes the early intervention and treatment components of the continuum of care, the major behavioral, pharmacological, and service components of care, services available, and emerging treatment technologies: $ Early Intervention, for addressing substance misuse problems or mild disorders and helping to prevent more severe substance use disorders. The goals of early intervention are to reduce the harms associated with substance misuse, to reduce risk behaviors before they lead to injury,18 to improve health and social function, and to prevent progression to a disorder and subsequent need for specialty substances use disorder services. Early intervention services may be considered the bridge between prevention and treatment services. For individuals with more serious substance misuse, intervention in these settings can serve as a mechanism to engage them into treatment. In 2015, an estimated 214,000 women consumed alcohol while pregnant, and an estimated 109,000 pregnant women used illicit drugs. Positive screening results should then be followed by brief advice or counseling tailored to the specifc problems and interests of the individual and delivered in a non-judgmental manner, emphasizing both the importance of reducing substance use and the individual’s ability to accomplish this goal. Professional organizations, including the American College of Obstetricians and Gynecologists, the American Medical Association, the American Academy of Family Physicians, and the American Academy of Pediatrics recommend universal and ongoing screening for substance use and mental health issues for adults and adolescents. Within these contexts, substance misuse can be reliably identifed through dialogue, observation, medical tests, and screening instruments. In addition to these tools, single-item screens for presence of drug use (“How many times in the past year have you used an illegal drug or used a prescription medication for nonmedical reasons? They often include feedback to the individual about their level of use relative to safe limits, as well as advice to aid the individual in decision-making. In such cases, the care provider makes a referral for a clinical assessment followed by a clinical treatment plan developed with the individual that is tailored to meet the person’s needs. The literature on the effectiveness of drug-focused brief intervention in primary care and emergency departments is less clear, with some studies fnding no improvements among those receiving brief interventions. Trials evaluating different types of screening and brief interventions for drug use in a range of settings and on a range of patient characteristics are lacking. Of those who needed treatment but did not receive treatment, over 7 million were women and more than 1 million were adolescents aged 12 to 17. The most common reason is that they are unaware that they need treatment; they have never been told they have a substance use disorder or they do not consider themselves to have a problem. This is one reason why screening for substance use disorders in general health care settings is so important. In addition, among those who do perceive that they need substance use disorder treatment, many still do not seek it. For these individuals, the most common reasons given are:19 $ Not ready to stop using (40. A common 1 clinical feature associated with substance use disorders is an individual’s tendency to underestimate See Chapter 2 - The Neurobiology of the severity of their problem and to over-estimate Substance Use, Misuse, and Addiction. This is likely due to 1 substance-induced changes in the brain circuits that control impulses, motivation, and decision making. The costs of care and lack of insurance coverage are particularly important issues for people with substance use disorders. However, even if an individual is insured, the payor may not cover some types or components of substance use disorder treatments, particularly medications. Harm reduction programs provide public health-oriented, evidence-based, and cost-effective services to prevent and reduce substance use-related risks among those actively using substances,59 and substantial evidence supports their effectiveness. Strategies include outreach and education programs, needle/syringe exchange programs, overdose prevention education, and access to naloxone to reverse potentially lethal opioid overdose. Outreach and Education Outreach activities seek to identify those with active substance use disorders who are not in treatment and help them realize that treatment is available, accessible, and necessary. Outreach and engagement methods may include telephone contacts, face-to-face street outreach, community engagement,64 or assertive outreach after a referral is made by a clinician or caseworker. Educational campaigns are also a common strategy for reducing harms associated with substance use. Such campaigns have historically been targeted toward substance-using individuals, giving them information and guidance on risks associated with sharing medications or needles, how to access low or no-cost treatment services, and how to prevent a drug overdose death. New cases of Hepatitis C infection increased 250 percent between 2010 and 2014, and occur primarily among young White people who inject drugs. The goal of needle/syringe exchange programs is to minimize infection transmission risks by giving individuals who inject drugs sterile equipment and other support services at little or no cost. Needle/syringe exchange programs also attempt to encourage individuals to engage in substance use disorder treatment. Overdose deaths from opioid pain relievers and heroin have risen dramatically in the past 14 years,80 from 5,990 in 1999 to 29,467 in 2014, and most were preventable. Rates of opioid overdose deaths are particularly high among individuals with an opioid use disorder who have recently stopped their use as a result of detoxifcation or incarceration. As a result, their tolerance for the drug is reduced, making them more vulnerable to an overdose. Those who mix opioids with alcohol, benzodiazepines, or other drugs also have a high risk of overdose. Rather, the effects develop gradually as the drug depresses a person’s breathing and heart rate. This gradual progress means that there is typically a 1- to 3-hour window of opportunity after a user has taken the drug in which bystanders can take action to prevent the user’s death. It works by displacing opioids from receptors in the brain, thereby blocking their effects on breathing and heart rate. The rising number of deaths from opioid overdose has led to increasing public health efforts to make naloxone available to at-risk individuals and their families, as well as to emergency medical technicians, police ofcers, and other frst responders, or through community-based opioid overdose prevention programs. Interventions that distribute take-home doses of naloxone along with education and training for those actively using opioids and their peers and family members, have the potential to help decrease overdose- related deaths. But by the time an overdosing person is reached and treated, it is often too late to save them. These programs have been shown to be an effective, as well as cost-effective, way of saving lives. To reverse these trends, it is important to do everything possible to ensure that emergency personnel, as well as at-risk opioid users and their loved ones, have access to lifesaving medications like naloxone. Acute Stabilization and Withdrawal Management Withdrawal management, often called “detoxifcation,” includes interventions aimed at managing the physical and emotional symptoms that occur after a person stops using a substance. Withdrawal symptoms vary in intensity and duration based on the substance(s) used, the duration and amount of use, and the overall health of the individual. Some substances, such as alcohol, opioids, sedatives, and tranquilizers, produce signifcant physical withdrawal effects, while other substances, such as marijuana, stimulants, and caffeine, produce primarily emotional and cognitive withdrawal symptoms. Most periods of withdrawal are relatively short (3 to 5 days) and are managed with medications combined with vitamins, exercise, and sleep.
The current dose recommendations resulted in similar day-7 lumefantrine plasma concentrations in all non-pregnant patients best buy for proventil asthmatic bronchitis 6 month, except for the smallest children (weighing 5–14 kg) order discount proventil line asthmatic bronchitis wiki. Because of dose-limited absorption cheap proventil 100 mcg with visa asthma treatment wiki, however, it is uncertain whether increases in individual doses would result in predictably higher lumefantrine exposure in these young children. Extended or more frequent dosing regimens should be evaluated prospectively in this age group. Clinical pharmacokinetics and pharmacodynamics and pharmacodynamics of artemether–lumefantrine. Comparable lumefantrine oral bioavailability when co-administered with oil- fortifed maize porridge or milk in healthy volunteers. Pharmacokinetic study of artemether–lumefantrine given once daily for the treatment of uncomplicated multidrug-resistant falciparum malaria. The effect of food consumption on lumefantrine bioavailability in African children receiving artemether–lumefantrine crushed or dispersible tablets (Coartem) for acute uncomplicated Plasmodium falciparum malaria. Supervised versus unsupervised antimalarial treatment with six-dose artemether–lumefantrine: pharmacokinetic and dosage-related fndings from a clinical trial in Uganda. Pharmacokinetic and pharmacodynamic characteristics of a new pediatric formulation of artemether–lumefantrine in African children with A uncomplicated Plasmodium falciparum malaria. Pharmacokinetics and pharmacodynamics of lumefantrine (benfumetol) in acute falciparum malaria. Population pharmacokinetics and pharmacodynamics of artemether and lumefantrine during combination treatment in children with uncomplicated falciparum malaria in Tanzania. Lefevre G, Looareesuwan S, Treeprasertsuk S, Krudsood S, Silachamroon U, Gathmann I, et al. A clinical and pharmacokinetic trial of six doses of artemether–lumefantrine for multidrug-resistant Plasmodium falciparum malaria in Thailand. Comparison of bioavailability between the most available generic tablet formulation containing artemether and lumefantrine on the Tanzanian market and the innovator’s product. Population pharmacokinetics of artemether, lumefantrine, and their respective metabolites in Papua New Guinean children with uncomplicated malaria. Effect of single nucleotide polymorphisms in cytochrome P450 isoenzyme and N-acetyltransferase 2 genes on the metabolism of artemisinin-based combination therapies in malaria patients from Cambodia and Tanzania. Population pharmacokinetics of mefoquine, piperaquine and artemether–lumefantrine in Cambodian and Tanzanian malaria patients. Multiple dose pharmacokinetics of artemether in Chinese patients with uncomplicated falciparum malaria. The pharmacokinetics of artemether and lumefantrine in pregnant women with uncomplicated falciparum malaria. A randomised controlled trial of artemether–lumefantrine versus artesunate for uncomplicated plasmodium falciparum treatment in pregnancy. Pharmacokinetic properties of artemether, dihydroartemisinin, lumefantrine, and quinine in pregnant women with uncomplicated Plasmodium falciparum malaria in Uganda. Population pharmacokinetics of artemether and dihydroartemisinin in pregnant women with uncomplicated Plasmodium falciparum malaria in Uganda. Population pharmacokinetics of lumefantrine in pregnant women treated with artemether–lumefantrine for uncomplicated Plasmodium falciparum malaria. Molecular and pharmacological determinants of the therapeutic response to artemether–lumefantrine in multidrug-resistant Plasmodium falciparum malaria. Effcacy of artemether–lumefantrine in area of high malaria endemicity in India and its correlation with blood concentration of lumefantrine. Treatment of acute uncomplicated falciparum malaria with artemether–lumefantrine in nonimmune populations: a safety, effcacy, and pharmacokinetic study. Population pharmacokinetics of lumefantrine in pregnant and nonpregnant women with uncomplicated Plasmodium falciparum malaria in Uganda. Update on the effcacy, effectiveness and safety of artemether–lumefantrine combination therapy for treatment of uncomplicated malaria. Desbutyl– lumefantrine is a metabolite of lumefantrine with potent in vitro antimalarial activity that may infuence artemether–lumefantrine treatment outcome. Effcacy and effectiveness of artemether–lumefantrine after initial and repeated treatment in children < 5 years of age with acute uncomplicated Plasmodium falciparum malaria in rural Tanzania: a randomized trial. Therapeutic effcacy of artemether–lumefantrine and 5 artesunate–mefoquine for treatment of uncomplicated Plasmodium falciparum malaria in Luang Namtha Province, Lao People’s Democratic Republic. Similar effcacy and tolerability of double-dose chloroquine and artemether–lumefantrine for treatment of Plasmodium falciparum infection in Guinea-Bissau: a randomized trial. Effcacy and safety of artemether–lumefantrine dispersible tablets compared with crushed commercial tablets in African infants and children with uncomplicated malaria: a randomised, single-blind, multicentre trial. Comparison of the cardiac effects of the antimalarials co-artemether and halofantrine in healthy participants. In vivo, artesunate is rapidly converted to its active metabolite dihydroartemisinin. H3C The mechanism of action of the artemisinin derivatives is not well-defned but involves cation-mediated generation of reactive intermediates and reduction of the peroxide bridge. Peak concentrations of artesunate are reached within a few minutes of parenteral administration; thereafter, artesunate is rapidly eliminated. There is no evidence that artemisinin derivatives are teratogenic in humans, but experience is still limited. While the possible risk for teratogenicity limits the use of artemisinin derivatives in the treatment of uncomplicated malaria in women in the frst trimester, treatment of severe malaria with artesunate is recommended as it is potentially life-saving A for the mother. Artesunate has been successfully and safely administered in the 5 second and third trimesters of pregnancy (1, 33). Adverse events Artesunate is generally well-tolerated and has a better safety profle than quinine in severe malaria (34–37). It has similar side-effects to other artemisinin derivatives, including hypersensitivity reactions (risk estimate, 1 in 3000), gastrointestinal disturbances, cough, rash, arthralgia, dizziness and delayed haemolysis. Clinically, the most signifcant effect is haemolysis, which has been reported up to weeks after treatment (38) (see section 7. Dose-dependent neutropenia was observed in Cambodia, where an oral dose of 6 mg/kg bw artesunate for 7 days resulted in signifcantly lower neutrophil counts than in those patients given 2 or 4 mg/kg bw (39). Other adverse effects observed in animal models, such as hepatotoxicity and neurotoxicity, have not been observed in clinical studies at therapeutic doses (40–42). Contraindications Artesunate is contraindicated in patients with known hypersensitivity to artesunate or artemisinin derivatives. Cautions As lower plasma concentrations of artesunate and dihydroartemisinin are reported in young children with severe anaemia, it is important to monitor their response to treatment closely. While use of artesunate in patients with renal or hepatic impairment has not been studied extensively, the limited data available (and the known metabolism and excretion of drug) do not suggest that artesunate would be toxic to renally or hepatically impaired individuals. Dosage optimization For the treatment of uncomplicated malaria, the target dose of artesunate remains 4 mg/kg bw daily, with a daily dose range of 2–10 mg/kg bw. Children weighing < 25 kg with severe malaria had lower exposure to intravenous or intramuscular artesunate and its active metabolite dihydroartemisinin than older children and adults given the same dose of 2. This may increase the risk for treatment failure, which can be fatal in severe malaria. These models confrmed that young children (< 25 kg/5 years) should receive a slightly higher dose of 3 mg/kg (see section 7.
Order proventil 100mcg with mastercard. ऊपर खिसकी नाभी या धरन ठीक करने का दुनिया का सबसे आसान अनोखा और जबरदस्त तरीका सीखें | Best for IBS.
If the side effects are alleviated buy discount proventil 100mcg online asthma definition quantitative, an attempt to gradually increase the dose again can be considered discount proventil 100mcg mastercard asthma definition 18th. The safety of the agent in the particular patient must be carefully evaluated before continuing with the medication once a side effect has been noted purchase proventil 100mcg fast delivery asthma 2015. Reasons that more than one medication, each from a different class of agents, might be prescribed include patients with complex comorbid conditions or those with partially-responsive 58,160 or treatment resistant cases. In clinical practice it is not unusual to have a patient on multiple psychotropic medications from different classes of drugs. It appears that a substantial number of hospitalized children and adolescents receive more than one psychotropic medication. Unfortunately, there are limited data regarding the long-term use of combinations of medications in youths. Due to the possibility of significant risks associated with these agents, the use of more than one agent is not recommended and is not supported in the scientific literature. While these medications fall within the same general class, it is clear they are not interchangeable. Significant differences in side effect profiles and mechanism of action exist and switching among these agents should be done with clear and precise reasoning reflective of current empirical data. Re-evaluation of the initial diagnosis, assessment for comorbid conditions, and the redefining of targeted symptoms may lead to try a trial of a different class of medication in these patients. Increased vigilance in the monitoring of the potential side effects is therefore needed, recognizing practical limitations. Obesity is associated with an increased risk of cardiovascular disease, diabetes, knee and joint injury, hyperlipidemia and hypertension. Developmentally normed growth charts can be found at the Center for Disease Control web site (www. There is also evidence to suggest that the 125 development of diabetes is not only directly related to weight gain. Therefore, careful monitoring for diabetes, through close attention to the clinical signs and symptoms of diabetes, and regular monitoring of blood glucose levels and, as needed, hemoglobin A1C is 121,161,162 warranted. Studies have shown that elevated lipid levels, even early in life, may have a role in the 134 development of cardiovascular disease throughout the lifespan. For patients whose family history is not available, particularly careful consideration regarding medication choice and monitoring is recommended. In youths who have significant weight changes, further evaluation or intervention should also be considered. As some of the most concerning short and long-term associated side effects with these agents are movement disorders, careful attention to their development is warranted. As the relationship between prolactin levels and clinical outcome has yet to be more precisely defined, prolactin measurement during antipsychotic pharmacotherapy does not appear to be warranted in the absence of possible prolactin-related side effects. Clozapine: Labeling for clozapine provides guidelines regarding the monitoring of hematological parameters for patients being treated with this agent. Although not developed for use in youths, per se, these monitoring parameters should be employed in children and adolescents treated with clozapine. For those patients who gain a substantive amount of weight, monitoring of liver enzymes should also be considered. Quetiapine: There are data from animals-based studies to suggest the possibility that quetiapine is associated with a risk of cataract formation. For this reason, a baseline ophthalmologic examination with periodic re-assessment is recommended by the manufacturer. The determination of treatment duration should be based on multiple factors including the severity of symptoms, the psychosocial settings, and the natural course of the illness being treated. Risks are associated with the abrupt discontinuation of these agents, including withdrawal dyskinesia. The abrupt withdrawal of a medication that has been ameliorating symptoms may also clinically destabilize a patient as a result of symptom exacerbations. Except in cases where a severe and/or dangerous side effect has developed, these agents should not be abruptly discontinued. As such, the parameters should not be deemed inclusive of all proper methods of care nor exclusive of other methods of care directed at obtaining the desired results. The ultimate judgment regarding the care of a particular patient must be made by the clinician in light of all of the circumstances presented by the patient and his or her family, the diagnostic and treatment options available, and available resources. National trends in the outpatient treatment of children and adolescents with antipsychotic drugs. A retrospective chart review of risperidone use in treatment- resistant children and adolescents with psychiatric disorders. Atypical antipsychotics in the treatment of children and adolescents: clinical applications. Physician specialty associated with antipsychotic prescribing for youths in Texas Medicaid Program. Trends in the use of typical and atypical antipsychotics in children and adolescents. Broadened use of atypical antipsychotic drugs: safety, effectiveness, and policy challenges. Prevalence of atypical antipsychotic drug use among commercially insured youths in the United States. Open-label, 8-week trial of olanzapine and risperidone for the treatment of bipolar disorder in preschool-age children. Diagnostic and Statistical Manual of Mental Disorders (Fourth Edition, Text Revision). Use of pharmacotherapy for insomnia in child psychiatry practice: a national survey. Phenomenology and epidemiology of childhood psychiatric disorders that may necessitate treatment with atypical antipsychotics. Benefit-risk assessment of atypical antipsychotic treatment of schizophrenia and comorbid disorders in children and adolescents. Childhood-onset schizophrenia: a double-blind, randomized clozapine-olanzapine comparison. Clozapine treatment of children and adolescents with bipolar disorder and schizophrenia: a clinical case series. Clozapine: its impact on aggressive behavior among children and adolescents with schizophrenia. Clozapine treatment of adolescents with posttraumatic stress disorder and psychotic symptoms. Risperidone for the core symptom domains of autism: results from the study by the Autism Network of the Research Units on Pediatric Psychopharmacology. Risperidone treatment of autistic disorder: longer-term benefits and blinded discontinuation after 6 months. A randomized, double-blind, placebo-controlled study of risperidone maintenance treatment in children and adolescents with disruptive behavior disorders.
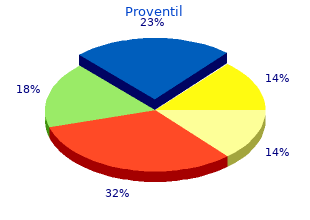
Ask patients specifc questions about attitudes safe 100mcg proventil asthma symptoms stomach pain, beliefs purchase 100mcg proventil visa asthma 49392, and cultural norms related to taking medications buy proventil line asthma definition and pathophysiology. Evaluate adherence Ask patients simply and directly whether they are sticking to their drug regimen. Executive Summary Non-adherence can threaten patients’ health individually as well as add vast costs to the health care system—an 1 estimated $290 billion annually. Non-adherence can threaten patients’ health individually as well as add vast costs to the health care system—an estimated $290 billion annually. This population represents 30 percent of all adults, with a 1 “Thinking Outside The Pillbox: A System-wide Approach to Improving Patient Adherence for Chronic Disease. The National Report Card on Adherence is based on an average of answers to questions on nine non-adherent behaviors. Whether or not, in the past 12 months, patients: • Failed to fill or refill a prescription; • Missed a dose; • Took a lower or higher dose than prescribed; • Stopped a prescription early; • Took an old medication for a new problem without consulting a doctor; • Took someone else’s medicine; or • Forgot whether they’d taken a medication. National Medication Adherence Report Card Average Grade: C+ A B 24% 24% F 15% C 20% D 16% 3 The score can range from 0 (non-adherence on all nine behaviors) to 100 (perfect adherence). Grouping adherence levels [see chart on previous page], just 24 percent earn an A grade for being completely adherent. An additional 24 percent are largely adherent, reporting one non-adherent behavior out of nine (a grade of B). Twenty percent earn a grade of C and 16 percent a D for being somewhat non-adherent, with two or three such behaviors in the past year, respectively. The remaining 15 percent—one in seven adults with chronic conditions—are largely non-adherent, with four or more such behaviors, an F grade. Survey results on a subject such as medication adherence can be influenced by potential reluctance among some respondents to admit to undesirable behaviors. Thus the grades in this survey, if anything, may understate non- adherence—underscoring cause for concern about the extent to which patients are following their medication instructions. In addition to self-reported adherence, the survey assessed demographic, attitudinal and behavioral factors related to prescription drug compliance, including individuals’ health and medical status; their ability to afford prescription medication; their feelings that their prescribed medications are safe, effective and easy to take; where they get their medications; and how informed they feel about their health, among other factors. Regression modeling, a statistical technique that assesses the independent strength of the relationship between two variables while holding other factors constant, identified the six key predictors of medication adherence. Those include—in order of magnitude: • Patients’ personal connection with a pharmacist or pharmacy staff; • How easy it is for them to afford their medications; • The level of continuity they have in their health care; • How important patients feel it is to take their medication exactly as prescribed; • How well informed they feel about their health; and • The extent to which their medication causes unpleasant side effects. These predictors, as well as other results of this survey, indicate a variety of avenues by which health care providers and pharmacists alike can address non-adherence—among them, better informing patients of the importance of adherence, strengthening a sense of personal connection and communication between patients/ caregivers and their health care and pharmacy providers and encouraging patients to discuss side effects with those providers. The survey also found demographic as well as attitudinal and informational differences in adherence: older Americans indicate greater adherence than younger respondents, for example, and those with lung problems report lower adherence than those without this chronic condition. When non-adherent respondents are asked their reasons for failing to comply with doctors’ orders, the most commonly mentioned reason is simply forgetting, cited by more than four in 10 as being a major reason. Other top reasons include running out of medication, being away from home, trying to save money and experiencing side effects. These, as well as further details about the drivers of medication adherence, are outlined in the full report. The survey was produced and analyzed, and this report written, by Langer Research Associates, of New York, N. The full report, including its appendices on methodology, statistical analyses and the full questionnaire and topline results, is available for download at www. Millions of adults age 40 and older with chronic conditions are departing from doctors’ instructions in taking their medications— skipping, missing or forgetting whether they’ve taken doses, failing to fll or refll prescriptions, under- or over-dosing or taking medication prescribed for a different condition or to a different person. An overall C+ grade underscores the problem; the F grades earned by one in seven of these medication users—the equivalent of more than 10 million adults—should heighten alarm. This survey not only establishes the breadth of the problem but evaluates factors that infuence medication non-adherence, suggesting paths to attempt to address the problem. Chief predictors of non-adherence include the presence or absence of a personal connection with a pharmacist or pharmacy staff; the affordability of prescribed medications; a belief in the importance of following instructions in taking medications; patients’ general levels of health information; and the presence of side effects. Pharmacists have a role at the forefront of addressing prescription medication non- Pharmacists have a role at the forefront of addressing prescription medication non-adherence. The results of this survey indicate that much depends on the extent to which pharmacists and pharmacy staff establish a personal connection with their patients and caregivers and engage with them to encourage fuller understanding of the importance of taking medications as prescribed. Independent pharmacists may be particularly well-placed to boost adherence, given their greater personal connection with patients. Health care providers have a vital role to play in stressing the importance of taking medications as prescribed, in monitoring and helping patients avoid or reduce unpleasant side effects that may compromise adherence and in helping to keep patients more generally well-informed about their health conditions. Health care providers, including pharmacists, can help reduce non-adherence by assisting economically vulnerable patients in finding the most affordable medication options. Better information, communication and patient/ caregiver support have been shown in previous studies to increase patients’ engagement and involvement in their health care, their satisfaction with their care and their loyalty to their health care providers. This survey shows yet another potential positive benefit of increased patient engagement—a reduction in the currently high levels of prescription medication non-adherence in the United States, and its associated costs and health risks alike. It is important that you, the patient, take responsibility in knowing which drugs you should try to avoid. Usually any T hearing problem will only be caused by exceeding the recommended dosage of the medications. If you are experiencing a hearing problem, or if there is a hearing disorder in your family, it is imperative that your treating physician and pharmacist be aware of this fact. If you are prescribed one of the medications found on this list, you should speak to your physician to see if another, potentially less toxic drug, could be used in its place. If the drug is over-the-counter, you should ask the pharmacist for a recommendation of a less toxic drug. In the lists that follow, the generic name of the drug is given first, with the trade name, if available, followed in parentheses and capitalized. The inclusion of a particular trade name and the exclusion of another should not be interpreted as prejudicial either for one nor against the other. When a solution Salicylates of an aminoglycoside antibiotic is used on • aspirin and aspirin- the skin together with an aminoglycoside containing products antibiotic used intravenously, there is a • salicylates and methyl- risk of an increase of the ototoxic effect, salicylates (linaments) especially if the solution is used on a (Toxic effects appear to be dose related wound that is open or raw, or if the and are almost always reversible once patient has underlying kidney damage. Hearing loss caused by this check with your doctor or pharmacist to class of antibiotics is usually permanent. The fact that – amikacin (Amakin) aminoglycosides and vancomycin are often – gentamycin (Garamycin) used together intravenously when treating – kanamycin (Kantrex) life-threatening infections futher exaggerates – neomycin (Found in many over-the- the problem. The League for the Hard of Hearing, founded in 1910, is a private not-for-profit rehabilitation agency for infants, children and adults who are hard of hearing, deaf, and deaf-blind. The mission of the League for the Hard of Hearing is to improve the quality of life for people with all degrees of hearing loss. This is accomplished by providing hearing rehabilitation and human service programs for people who are hard of hearing and deaf, and their families, regardless of age or mode of communication. We strive to empower consumers and professionals to achieve their potential and to provide leadership to, and be the model for, disciplines that relate to hearing rehabilitation.