


University of Wisconsin-Eau Claire. U. Flint, MD: "Purchase Micardis online - Effective Micardis OTC".
In addition order micardis 80 mg visa blood pressure percentile, uncontrolled vomiting can produce dehydration order micardis 20 mg mastercard blood pressure medication verapamil, profound metabolic imbalances discount micardis 40mg visa blood pressure chart low bp, and nutrient depletion. Mechanisms that trigger vomiting Two brainstem sites have key roles in the vomiting reflex pathway. Thus, it can respond directly to chemical stimuli in the blood or cerebrospinal fluid. The second important site, the vomiting center, which is located in the lateral reticular formation of the medulla, coordinates the motor mechanisms of vomiting. Often, the color or smell of3 chemotherapeutic drugs (and even stimuli associated with chemotherapy) can activate higher brain centers and trigger emesis. Antiemetic drugs Considering the complexity of the mechanisms involved in emesis, it is not surprising that antiemetics represent a variety of classes (ure 40. Prochlorperazine is effective against low or moderately emetogenic chemotherapeutic agents (for example, fluorouracil and doxorubicin). Although increasing the dose improves antiemetic activity, adverse effects are dose limiting. These drugs can be administered as a single dose prior to chemotherapy (intravenously or orally) and are efficacious against all grades of emetogenic therapy. Ondansetron and granisetron prevent emesis in 50% to 60% of cisplatin-treated patients. These agents are also useful in the management of postoperative nausea and vomiting. Antidopaminergic adverse effects, including extrapyramidal symptoms, limit long-term high-dose use. Metoclopramide enhances gastric motility and is useful for patients with gastroparesis. Droperidol had been used most often for sedation in endoscopy and surgery, usually in combination with opioids or benzodiazepines. Their beneficial effects may be due to their sedative, anxiolytic, and amnestic properties (see Chapter 9). Their antiemetic mechanism is not known, but it may involve blockade of prostaglandins. Therefore, it may affect the metabolism of other drugs that are substrates of these isoenzymes and is subject to numerous drug interactions. Combination regimens Antiemetic drugs are often combined to increase efficacy or decrease toxicity (ure 40. Antihistamines, such as diphenhydramine, are often administered in combination with high-dose metoclopramide to reduce extrapyramidal reactions or with corticosteroids to counter metoclopramide-induced diarrhea. Antidiarrheal drugs include antimotility agents, adsorbents, and drugs that modify fluid and electrolyte transport (ure 40. They activate presynaptic opioid receptors in the enteric nervous system to inhibit acetylcholine release and decrease peristalsis. Loperamide is used for the general treatment of acute diarrhea, including traveler’s diarrhea. Because these drugs can contribute to toxic megacolon, they should not be used in young children or in patients with severe colitis. Presumably, these agents act by adsorbing intestinal toxins or microorganisms and/or by coating or protecting the intestinal mucosa. They are much less effective than antimotility agents, and they can interfere with the absorption of other drugs. Agents that modify fluid and electrolyte transport Bismuth subsalicylate, used for prevention and treatment of traveler’s diarrhea, decreases fluid secretion in the bowel. Laxatives Laxatives are commonly used in the treatment of constipation to accelerate the motility of the bowel, soften the stool, and increase the frequency of bowel movements. Laxatives increase the potential for loss of pharmacologic effect of poorly absorbed, delayed- acting, and extended-release oral preparations by accelerating their transit through the intestines. Its active ingredient is a group of sennosides, a natural complex of anthraquinone glycosides. In combination products with a docusate-containing stool softener, it is useful in treating opioid-induced constipation. Bisacodyl Available as suppositories and enteric-coated tablets, bisacodyl [bis-ak-oh-dil] is a potent stimulant of the colon. Castor oil This agent is broken down in the small intestine to ricinoleic acid, which is very irritating to the stomach and promptly increases peristalsis. Pregnant patients should avoid castor oil because it may stimulate uterine contractions. Bulk laxatives the bulk laxatives include hydrophilic colloids (from indigestible parts of fruits and vegetables). They form gels in the large intestine, causing water retention and intestinal distension, thereby increasing peristaltic activity. They should be used cautiously in patients who are immobile because of their potential for causing intestinal obstruction. Psyllium can reduce the absorption of other oral drugs, and administration of other agents should be separated from psyllium by at least two hours. Saline and osmotic laxatives Saline cathartics, such as magnesium citrate and magnesium hydroxide, are nonabsorbable salts (anions and cations) that hold water in the intestine by osmosis. This distends the bowel, increasing intestinal activity and producing defecation in a few hours. Oral doses reach the colon and are degraded by colonic bacteria into lactic, formic, and acetic acids. This increases osmotic pressure, causing fluid accumulation, colon distension, soft stools, and defecation. Lactulose is also used for the treatment of hepatic encephalopathy, due to its ability to reduce ammonia levels. Stool softeners (emollient laxatives or surfactants) Surface active agents that become emulsified with the stool produce softer feces and ease passage of stool. They may take days to become effective and are often used for prophylaxis rather than acute treatment. Stool softeners should not be taken concomitantly with mineral oil because of the potential for absorption of the mineral oil. Lubricant laxatives Mineral oil and glycerin suppositories are lubricants and act by facilitating the passage of hard stools. Mineral oil should be taken orally in an upright position to avoid its aspiration and potential for lipid or lipoid pneumonia. Also, drug–drug interactions are minimal because metabolism occurs quickly in the stomach and jejunum. Diet and psychosocial modifications play an important role in management of the disease, as well as drug therapy (ure 40. It may extend continuously to affect other parts of the colon, and is characterized by inflammation limited to the mucosal layer (ure 40.
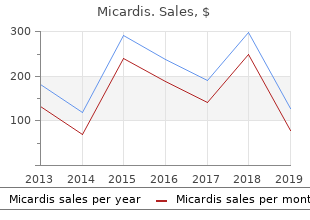
Diseases
Following fasciotomy purchase 20mg micardis free shipping blood pressure chart age 35, closure of the fascia is not indicated and skin closure should be undertaken cautiously discount micardis 80 mg overnight delivery hypertension guidelines aha. It is imperative to verify that all compartments of the affected extremity have been released discount 20 mg micardis with visa arteria jugularis, regardless of the surgical approach utilized. Anatomy may be distorted due to fracture deformity, excessive hematoma, or soft tissue avulsion, and it occasionally can be difficult to discern fascial planes. Negative-pressure wound therapy devices may also be beneficial for promoting growth of granulation tissue within a fasciotomy bed, in anticipation of skin grafting, or in maintaining smaller wound dimensions, in anticipation of delayed primary closure [134,135]. Risk can be minimized by careful and meticulous dissection technique, maintaining nerves and vessels within a cutaneous flap (if possible), and assuring that neither is directly exposed to the environment (dressing) at the conclusion of the case. At least one case of profound hemorrhage after erosion of an artery beneath a negative-pressure wound therapy device has been reported [136]. Analysis of long-term outcomes related to fasciotomy is difficult in the trauma setting due to the concomitant injuries that have invariably occurred and which can have an effect upon function. Nevertheless, a retrospective analysis of 40 patients undergoing leg fasciotomy for a variety of reasons has been published [137]. Complications of leg fasciotomy were common, and included neurological injury, hemorrhage, and infection. Another report indicated frequent patient complaints related to fasciotomy wounds, including decreased sensation, tethering of tendons, and recurrent ulceration [138]. Other known side effects of compartment release include pruritus, reflex sympathetic dystrophy, temperature sensitivity, venous stasis, and chronic edema. Despite these concerns, the morbidity and potential mortality of an untreated compartment syndrome is likely to be much higher. These reports, however, require cautious interpretation for their application to trauma, as they did not include patients who required fasciotomy for trauma-related compartment syndrome. As there are not any high-quality studies that dictate practice guidelines, the Orthopedic Trauma Association put together the recommendations based on expert opinion [145]. While these are current expert recommendations, the panel recommended that further high- quality studies are required [145]. Typical neurological injuries include radial nerve palsies in association with humeral shaft fractures, sciatic nerve palsies (peroneal branch, in particular) in association with pelvic and acetabular fractures, and brachial plexopathies in association with scapulothoracic dissociation. An early description of radial nerve palsy in association with humeral shaft fracture was published by Holstein and Lewis, and describes the association with a spiral fracture of the humeral shaft located at the junction between the middle and distal one-thirds of the diaphysis [147]. The radial nerve supplies motor innervation to the extensors of the hand and wrist; patients with radial nerve motor palsies will lack the ability to extend the wrist or hyperextend the interphalangeal joint of the thumb, which is mediated by the extensor pollicis longus. The interphalangeal joints of the fingers (index, long, ring, and small) are extended by the intrinsic muscles of the hand, which are innervated by the median and ulnar nerves, and therefore are not affected by radial nerve palsy. Radial nerve–mediated sensation includes the dorsal surfaces of the forearm and hand; the most specific location for radial nerve sensation is the dorsum of the first web space on the hand. Most radial nerve palsies are thought to be traction injuries (neurapraxias), as opposed to complete disruptions (neurotmesis) or impalings on bone edges [146]. Rarely, the radial nerve may become entrapped within the humeral fracture site, creating neurological deficits [118]. In the setting of high-velocity penetrating injury (gunshot wounds), a radial nerve palsy may be secondary to blast effect of the projectile (as opposed to nerve transaction). Radial nerve palsy at presentation of a patient with a humeral shaft fracture is not considered an indication for surgery, either for nerve exploration or humeral shaft fracture fixation. In the past, humeral shaft fracture patients presenting with intact radial nerve function which then is lost after manipulation of the fracture (e. Humeral shaft fracture fixation should be undertaken for patients who would benefit (or who specifically request fixation), after thorough risk and benefit discussions with the patients and/or their families, and should not be prompted by the presence of a radial nerve deficit. Electromyography and nerve conduction studies are not helpful in the acute setting, and have low sensitivity and specificity regarding the etiology of radial nerve palsy immediately after injury. Ultrasonic examination, however, can be beneficial to detect nerve laceration or entrapment, when utilized by experienced practitioners [148]. Splinting and occupational therapy, with daily manual stretching exercises, are beneficial to minimize this problem. Electromyography and nerve conduction studies may be performed between 6 and 12 weeks following the onset of the radial nerve palsy if there has been absolutely no recovery of function after the injury [146]. Therefore, an injury to the radial nerve at the midshaft of the humerus should be expected to result in dorsal hand sensory deficits for many weeks. Acetabular fractures with posterior dislocation of the hip have an association with the development of sciatic nerve palsy [150]. Pelvic or acetabular fractures, with extensions of fracture lines into the sciatic buttress at the greater sciatic notch, can result in direct laceration of the sciatic nerve; this pattern of fracture can also result in catastrophic hemorrhage due to laceration of the superior and/or inferior gluteal arteries. Pelvic ring disruptions, with wide displacement of the hemipelvis, can also cause sciatic nerve palsies or lumbosacral plexopathies [151], perhaps due either to avulsion of nerve roots or to neurapraxia [152,153]. The peroneal division of the sciatic nerve is more commonly affected than the tibial division [155]; it has been postulated that this has to do with more points at which the peroneal nerves are tethered down the lower extremity than the tibial nerves. Prognosis of these, however, is poorer than that for radial nerve palsy, perhaps secondary to the long distance across which recovery must occur (the nerve bud must travel from the pelvis to at least the superior leg, where innervation of the peroneal muscles and ankle and toe dorsiflexors occurs) [155]. Electromyography and nerve conduction studies are useful for characterizing the injury, and many patients with mild injuries regain good function [156]. Scapulothoracic dissociation, likened to a closed forequarter amputation [157], occurs when the shoulder girdle and upper extremity are pulled away from the midline [158]. Significant degrees of scapulothoracic dissociation can result in the rupture of subclavian or axillary vessels [157,159]. The injury complex can have devastating effects upon the neurological function of the upper extremity, due to the stretch of nerves or brachial plexus, or due to the avulsion of nerve roots from the cervical spine [157]. Degree of neurological injury and prognosis for recovery correlates with the location of vascular injury; more proximal vascular injury correlates with more severe neurological compromise and poorer prognosis [160]. Evidence of expanding hematoma within the axilla of a patient with such an injury should prompt emergent vascular surgical consultation. Careful attention to the vascular status of the distal upper extremity must be paid to any patient with a distracted clavicular fracture, a significantly displaced scapular fracture, or a clear increase in distance on anteroposterior chest radiograph between the thoracic spine and the medial border of the scapula, known as the scapular index [161]. Recovery of brachial plexus function after scapulothoracic dissociation is unreliable at best, especially after nerve root avulsion [159,160,162]. Bhattacharyya T, Mehta P, Smith M, et al: Routine use of wound vacuum-assisted closure does not allow coverage delay for open tibia fractures. Johansen K, Daines M, Howey T, et al: Objective criteria accurately predict amputation following lower extremity trauma. Ghaemmaghami V, Sperry J, Gunst M, et al: Effects of early use of external pelvic compression on transfusion requirements and mortality in pelvic fractures. Smith W, Williams A, Agudelo J, et al: Early predictors of mortality in hemodynamically unstable pelvis fractures.
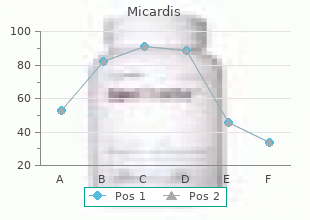
Diseases
Withdrawal bleeding is not a desired experience for many women order micardis 20 mg free shipping arrhythmia technologies institute, and today order discount micardis on line blood pressure 10, monthly bleeding cheap micardis 20 mg free shipping blood pressure phobia, periodic bleeding, or no bleeding are choices available for women. Any combination oral contraceptive can be used on a daily continuous dosing basis; even the lowest estrogen dose formulations pro- vide excellent bleeding and side efect profles in a continuous regimen. Occasionally, patients would like to postpone a menstrual period; for example, for a wedding, holiday, or vacation. Simply start a new package of pills the next day afer fnishing the series of active pills in the previous package. Using an electronic monitor- ing device to measure compliance, it was apparent that consistency of pill taking is even worse than what patients report; only 33% of women were documented to have missed no pills in cycle 1, and by cycle 3, about one third of the women missed three or more pills with many episodes of con- secutive days of missed pills. If a woman misses one pill, she should take that pill as soon as she remem- bers and take the next pill as usual. If she misses two pills in the frst 2 weeks, she should take two pills on each of the next 2 days; it is unlikely that a backup method is needed, but the ofcial consensus is to recommend backup for the next 7 days, especially if the missed pills occurred in the frst week. If the patient is using an oral contraceptive with 20 mg or less of estrogen and the missed pills occur in the frst week, consider the use of emergency contraception. A Clinical Guide for Contraception If two pills are missed in the third week, or if more than two active pills are missed at any time, another form of contraception should be used as backup immediately and for 7 days; if a Sunday starter, keep taking a pill every day until Sunday, and on Sunday start a new package; if a non-Sunday starter, start a new package the same day. One study demonstrated that skipping four consecutive pills at varying times in the cycle did not result in ovulation. Despite greater follicular activity with the lowest-dose oral contraceptives, ovulation is still efectively prevented. Although the progestational efects on endometrium and cervical mucus serve to ensure good contraceptive efcacy,97 conservative advice regarding missing pills is the safest message to convey. The most prevalent problems that can be identifed associated with appar- ent oral contraceptive failures are vomiting and diarrhea. Terefore, on starting oral contraception, patients need to be fully informed about breakthrough bleeding. Tere are two characteristic breakthrough bleeding problems: irregular bleeding in the frst few months afer starting oral contraception, and unex- pected bleeding afer many months of use. Efort should be made to manage A Clinical Guide for Contraception the bleeding problem in a way that allows the patient to remain on low-dose oral contraception. Tere is no evidence that the onset of bleeding is asso- ciated with decreased efcacy, no matter what oral contraceptive formu- lation is used, even the lowest dose products. Indeed, in a careful study, breakthrough bleeding did not correlate with changes in the blood levels of the contraceptive steroids. The incidence is greatest in the frst 3 months, rang- ing from 10% to 30% in the frst month to less than 10% in the third. Break- through bleeding rates are higher with the lowest dose oral contraceptives, but not dramatically. The basic pattern is the same, high- est in the frst month and a greater prevalence in smokers, especially in later cycles. Breakthrough bleeding is best managed by good educational anticipatory preparation of the patient at initiation of treatment, with encouragement and reassurance when bleeding occurs. It is helpful to explain to the patient that this bleeding represents tis- sue breakdown as the endometrium adjusts from its usual thick state to the relatively thin state allowed by the hormones in oral contraceptives. Breakthrough bleeding that occurs afer many months of oral contra- ceptive use is a consequence of the progestin-induced decidualization. This endometrium and the blood vessels within the endometrium tend to be fragile and prone to breakdown and asynchronous bleeding. Tere are two recognized factors (both preventable) that are associated with a greater incidence of breakthrough bleeding. Consistency of use and smoking increase spotting and bleeding, but inconsistency of pill taking is more important and has a greater efect in later cycles, whereas smoking exerts a general efect at any time. Young women who smoke are more likely to discontinue oral contraception,507 and this may be partly due to irregular bleeding. Cervical infection can be another cause of breakthrough bleeding; the prevalence of cervical chlamydial infections is higher among oral contracep- tive users who report breakthrough bleeding. If break- through bleeding is prolonged or if it is aggravating for the patient, regard- less of the point in the pill cycle, control of the bleeding can be achieved with a short course of exogenous estrogen. Usually, one course of estrogen solves the problem, and recurrence of bleeding is unusual (but if it does recur, another 7-day course of estrogen is efective). Remember that there is a signifcant reduction in the number of bleed- ing and spotting days, as well as the amount of withdrawal bleeding, in women using a 24-day regimen. Studies comparing 24- and 21-day regi- mens have indicated that some of the breakthrough bleeding experienced by women on 21-day regimens is due to follicular growth, a rise in endog- enous estrogen levels, followed by demise of the follicle and estrogen withdrawal bleeding. Tere are two operative mechanisms, therefore, in breakthrough bleeding: progestin-induced atrophic endometrium with vascular fragility and withdrawal bleeding in response to the rise and fall of endogenous estrogen levels associated with follicular growth and demise. Breakthrough bleeding in women using steroid contraception without a break, daily continuous dosing of oral contraceptives, is best treated by dis- continuing medication for 3 or 4 days (no more than once every 3 weeks), allowing a withdrawal menstrual sloughing. The progestin component of the pill will always domi- nate; hence, doubling the number of pills will also double the progestational impact and its decidualizing, atrophic efect on the endometrium and its destabilizing efect on endometrial blood vessels. Breakthrough bleeding, in our view, is not suf- cient reason to expose patients to the increased risks associated with higher dose oral contraceptives. Any bleeding that is not handled by this routine requires investigation for the presence of pathology. Tere is no evidence that any oral contraceptive formulations that are approximately equivalent in estrogen and progestin dosage are signifcantly diferent in the rates of breakthrough bleeding. Clinicians ofen become impressed that switching to another product efectively stops the break- through bleeding. It is more likely that the passage of time is the responsible factor, and bleeding would have stopped regardless of switching and regard- less of product. Amenorrhea With low-dose pills, the estrogen content is not sufcient in some women to stimulate endometrial growth. The progestational efect dominates to such a degree that a shallow atrophic endometrium is produced, lacking sufcient tissue to yield withdrawal bleeding. It should be emphasized that perma- nent atrophy of the endometrium does not occur, and resumption of normal ovarian function will restore endometrial growth and development. Indeed, A Clinical Guide for Contraception there is no harmful, permanent consequence of amenorrhea while on oral contraception. The major problem with amenorrhea while on oral contraception is the anxiety produced in both patient and clinician because the lack of bleeding may be a sign of pregnancy. The patient is anxious because of the uncertainty regarding pregnancy, and the clinician is anxious because of the medicolegal concerns stemming from the old studies, which indicated an increased risk of congenital abnormalities among the ofspring of women who inadver- tently used oral contraception in early pregnancy. We reviewed this prob- lem earlier, and emphatically stated that there is no association between oral contraception and an increased risk of congenital malformation, and there is no increased risk of having abnormal children. It is important to alert patients upon starting oral contraception that diminished bleeding and possibly no bleeding may ensue. A pregnancy test will allow reliable assessment for the presence of pregnancy even at this early stage. However, routine, repeated use of such testing is expensive and annoy- ing, and may lead to discontinuation of oral contraception. Many women are reassured with an understanding of why there is no bleeding and are able to continue on the pill despite the amenorrhea.